An animal model of HLA-independent, chimeric antigen receptor-mediated adoptive immunotherapy against cytomegaloviruses
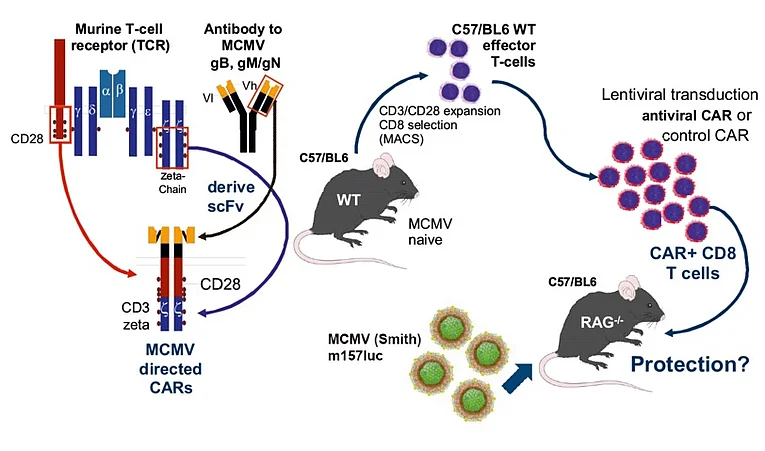
A great risk for immunosuppressed patients (i.e. during an allogeneic stem cell transplantation) as well as for immunocompromised people is an infection or reactivation of the human cytomegalovirus (HCMV). In immunocompetent individuals the immune system suppresses the spread of HCMV during an infection, resulting in an asymptomatic or mild course of the disease. Via various mechanisms, HCMV is able to deter a potent T cell response, which is crucial for an efficient control of the viral infection. This work investigates the effect of a potential immunotherapy with cytotoxic T cells expressing chimeric antigen receptors (CARs) on murine cytomegalovirus (MCMV) infection in the mouse model. CARs consist of a single chain variable fragment (scFv) derived from antibodies recognising viral glycoproteins (gB, gH, gN) on the surface of CMV-infected cells, coupled with a costimulatory domain (CD28 or 4-1BB) and the zeta-chain of the murine T cell receptor (CD3ζ) as activating domain (Figure, left). By means of an HLA-independent mechanism, CAR+ T cells are supposed to recognise viral glycoproteins on MCMV-infected cells, leading to an activation of the T cells, which results in the lysis of infected cells. In a previous project, Full et al. generated a HCMV-gB specific CAR and showed its efficacy in in vitro studies. In this project, various CAR constructs directed against different MCMV-specific glycoproteins will be generated. Afterwards, tests on expression, activation, cytokine secretion and cytotoxic effects will be conducted in human and murine cell lines. Finally, the most potent CAR constructs from the in vitro studies will be transduced into cytotoxic T cells, which will be administered to immunodeficient RAG-/- mice infected with a luciferase-expressing MCMV-reporter strain (MCMVm157luc). Tests on the optimal efficacy dose, the ideal administration time, the combination of T cells carrying different CARs, as well as the administration of human T cells carrying human CARs will be conducted (Figure, right).